Oncology medical billing is the process of submitting claims to insurance companies or other payers for oncology-related billing services associated with cancer management. The process involves verifying the patient’s coverage, accurately documenting medical history, submitting claims promptly, and ensuring compliance with regulations. Oncology medical billing requires understanding medical coding to run a successful oncology practices.
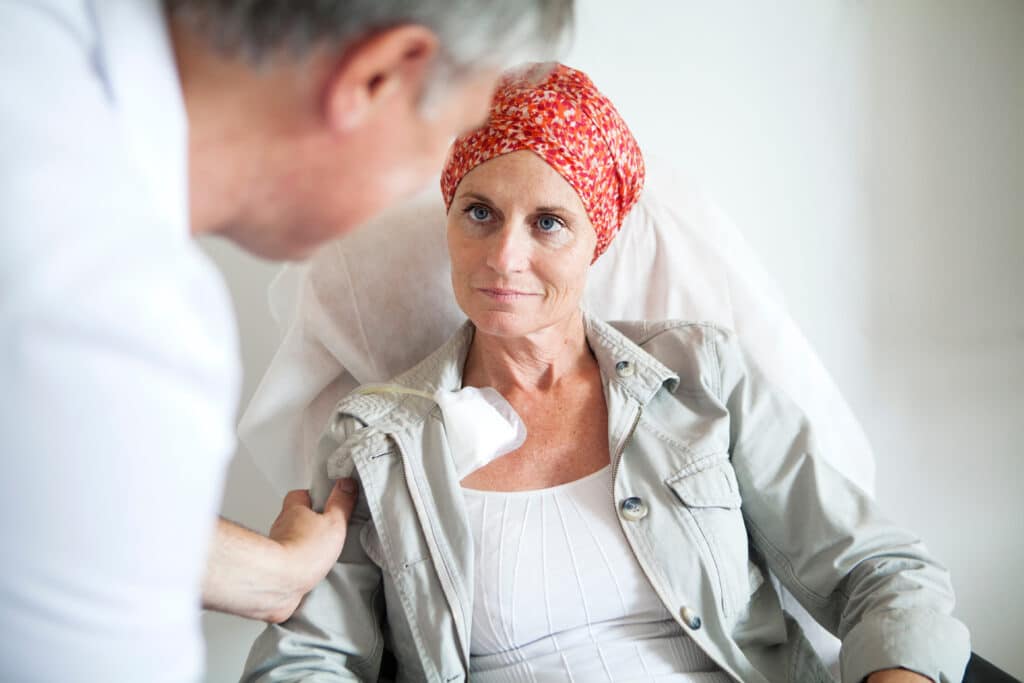
What is Oncology Medical Billing?
Oncology medical billing is a complex system that involves precise coding and documentation to ensure that healthcare organizations receive appropriate reimbursement for cancer treatment services. This specialized branch of medical billing takes into account the unique challenges that come with treating cancer patients, including the use of costly diagnostic tests, chemotherapy, and radiation therapy.
It requires a deep understanding of medical terminology and billing codes, as well as a commitment to staying up-to-date with changes in healthcare regulations and insurance policies. Cancer patients and their loved ones rely on the expertise of trained oncology medical billers to help them navigate the financial complexities of cancer treatment and ensure that they can access the care they need.
Importance of Accurate Billing in Oncology Practices
Accurate billing is essential in oncology practices, not just for administrative purposes, but also for ensuring patient satisfaction and ultimately, the quality of care they receive. With a growing emphasis on value-based care, coding errors or incomplete documentation can result in denied claims or underpayment, impacting the financial sustainability of the practice.
In addition, billing inaccuracies can cause unnecessary stress and frustration for patients, who may already be dealing with a challenging diagnosis.
Oncology Billing Codes: Understanding the Basics
In oncology billing, a variety of codes are used. Current Procedural Terminology (CPT) are codes used to describe medical procedures. International Classification of Diseases (ICD) codes that detail diagnoses.
Accurate medical coding is critical to getting paid for oncology services rendered. Here are just a few CPT codes and their meaning:
Accurate medical coding is critical to getting paid for oncology services rendered. Here are just a few CPT codes and their meaning:
- 77261–77299 — The work that goes into planning and preparing for radiation therapy, such as creating a personalized treatment plan and ensuring that the radiation delivery is to the correct body area
- 77600–77615 — Radiation therapy with hyperthermia, which is a treatment that involves using both radiation and heat to treat cancerous tumors
- 96401–96417 — The administration of chemotherapy and other complex drugs or biological agents through injection or intravenous infusion
In the oncology billing process, verifying insurance coverage and benefits is crucial. Determining the scope of the services needed before they begin can establish if the patient is responsible for any out-of-pocket expenses and, if so, how much. It can help avoid any surprises later regarding payment.
Accurate documentation of the patient’s medical history, examination, and treatment is crucial for oncology billing, including tracking all CPT and diagnosis codes. This is particularly important when dealing with complex cases involving multiple specialists, such as dermatologists. Using the best medical billing software with medical billers’ help, including those with expertise in oncology sub-specialties, is vital to automation.

Oncology Billing Workflow Steps
Navigating the complex world of oncology billing may seem daunting at first, but with a solid understanding of the necessary workflow steps, you can approach this process with confidence.
- Insurance Eligibility: Verify insurance coverage and obtain pre-authorization to confirm the patient’s health plan covers treatments and predictable payments. Accurate patient records and monitoring insurance changes are crucial.
- Capturing Charges: Accurately document all oncology billing services, including ICD and CPT codes and modifiers. Ensure timely capture of all charges and prevent missed or lost payments to avoid revenue loss.
- Claims Submission: Present the claims to the insurance company for payment, confirming they are accurate, complete, and delivered promptly to avoid delays. Review any rejections, appealing if necessary.
- Payment: The medical practice will receive compensation upon receipt of the processed insurance claim. Monitoring expenses, addressing outstanding balances, and maintaining accurate financial records while staying up to date on reimbursement rate changes are crucial.
- Data Reporting: Record critical metrics related to the billing oncology process, including tracking revenue, accounts receivable, and denials or rejections. The data can help identify areas for improvement and create an optimized invoicing process.
Challenges of Oncology Medical Billing
Oncology medical billing is a complex process prone to some challenges, specifically the medical coding and the frequent changes to these codes. A lack of understanding can lead to under-coding, errors, and denials, resulting in significant financial losses.
Misunderstanding codes can also cause payment delays, leading to frustration and delays in patient care. Staying current on code changes and training the billing oncology staff on proper coding practices is crucial to guarantee accuracy and minimize errors.
Tracking all billing services and oncology procedures can also be burdensome, but outsourcing to a professional medical coding and billing company can help streamline and automate the process.

Tips for Streamlining Oncology Medical Billing
Simplifying medical billing oncology from start to finish can be daunting. Here are several tips to ensure a smooth billing process and maximize repayment.
Understanding the Coding System
Healthcare professionals can improve their understanding of oncology coding by attending seminars, reading industry publications, and training with organizations like the American Academy of Professional Coders (AAPC). AAPC offers certification programs for medical coders to enhance their skills and accuracy. AAPC-certified professionals are highly skilled and valuable assets in the oncology medical billing process.
Working closely with medical billing professionals is helpful, as they have specialized knowledge in coding and billing. They can provide guidance on coding best practices, identify areas for improvement, and offer training and support as needed.
Many online resources, such as the Centers for Medicare and Medicaid Services (CMS), provide information on coding guidelines, regulations, and updates. By staying informed and operating with experts, healthcare providers can ensure their practices are accurate and compliant, improving reimbursement and overall financial success.
Verify Insurance Coverage
Contact the insurance company directly or use an online verification system to understand the patient’s benefits, co-pays, and deductibles plus avoid any surprises or unexpected expenses for the patient. Discuss any issues by completing this process before the patient’s visit.
Verifying health coverage can also reduce claim denials and delays. If the patient’s insurance information is not correct, this can result in a refused claim, which can be time-consuming to fix. By confirming health benefits early in the process, you can certify that all necessary information is accurate and up to date.
Accurate Documentation
Incomplete or wrong patient information can lead to claim rejections or interruptions, resulting in a loss of revenue for oncology practices. Ensure that precise documentation is recorded in the patient’s electronic health record (EHR) system, including the patient’s medical history.
Medical professionals must record all diagnoses, treatment plans, and tests or procedures. Keeping track of all the codes used during the encounter is essential to creating accurate and complete claims for submission. By confirming that all the data is correct, healthcare providers can reduce the number of claim rejections, resulting in faster payment and improved cash flow.
Timely Submission
Failure to submit timely statements can result in compensation delays and even denials. Insurance companies typically have strict deadlines for accepting claims, and missing these targets can cause significant economic loss.
Providers can ensure that claims are accepted promptly and efficiently by implementing a claims tracking system and monitoring submission deadlines. The result is timely service reimbursement and reduced monetary strain on the practice. This process of tracing also helps streamline the billing process.
Stay Updated with Regulations
The healthcare industry constantly evolves, introducing new regulations and policies. Medical providers must stay informed of the latest medical billing oncology landscape changes to confirm compliance with the rules. Failure to stay up-to-the-minute with regulations can result in legal repercussions.
Healthcare organizations must allocate time and resources to stay educated and updated on guideline changes, which can involve attending industry conferences, reviewing updates from governing bodies, and frequently studying internal billing processes to guarantee they align with present-day parameters. By staying current with the coding, medical providers can reduce errors and avoid costly consequences.
Use Technology
Technology like EHR systems allows healthcare teams to access and manage patient health information efficiently. EHRs can also submit claims and verify insurance coverage, leading to quicker reimbursements.
Medical billing software can also help program claim submission, payment posting, and denial management. This automation saves time, allowing healthcare providers to focus on providing quality care to patients. Integrated digital charge capture solutions can help eliminate missed or lost charges by providing access to real-time billing and coding information.
These solutions also share critical patient information seamlessly, which can improve patient outcomes. Healthcare providers can streamline oncology billing guidelines by using technology for effective revenue cycle management.
Hire a Professional Medical Billing Company
Managing invoicing in-house can be challenging, especially for small healthcare providers with limited resources. Outsourcing to a professional medical coding and billing company is a smart option, as their oncology billing specialists are experts in the latest billing regulations and technology. They handle all aspects of invoicing, from claims submission to follow-up, and confirm that client practices are reimbursed for all oncology billing services.
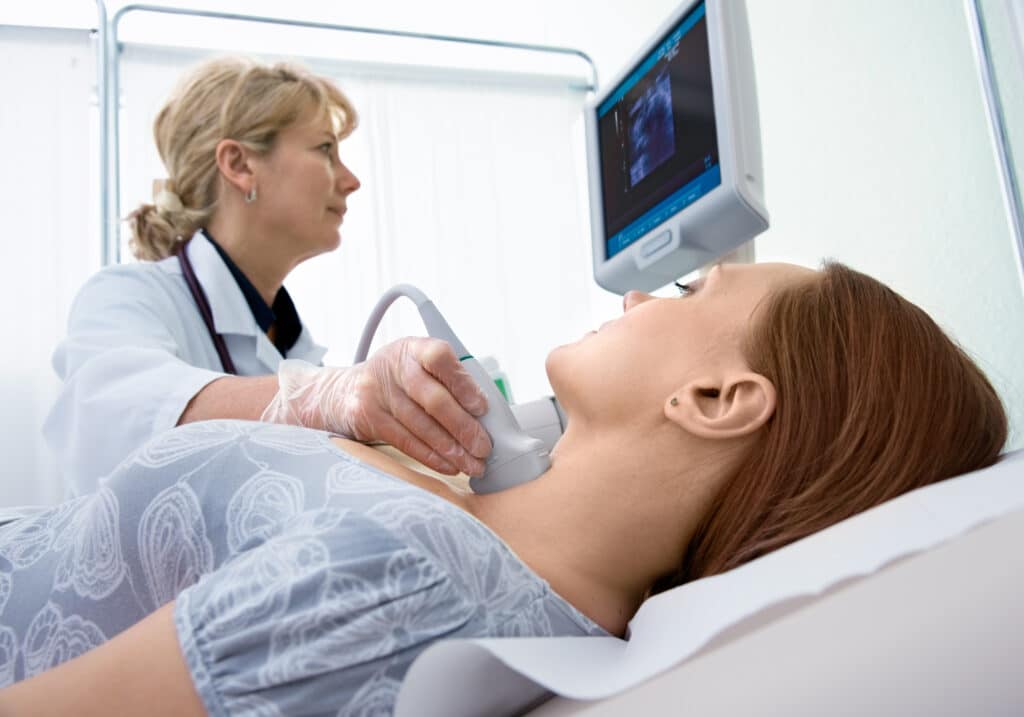
Oncology Billing Software
Outsourcing oncology medical billing saves time that can be better utilized in patient care. It can also diminish mistakes and improve collections, as professional billing companies typically use the latest technology to maximize accuracy and efficiency. Finding the best medical billing software solution guarantees you are smoothly and competently following oncology billing guidelines.
CollaborateMD is a medical billing company offering end-to-end practice management solutions. The cloud-based platform streamlines invoicing workflows and reduces manual errors, allowing healthcare providers to focus on patient care instead of administrative tasks. With CollaborateMD, medical professionals can easily manage patient data, claims submissions, and payments while ensuring compliance with industry regulations.
CollaborateMD is intuitive and user-friendly, with a customizable dashboard that allows staff to easily track important metrics, such as outstanding claims and payments received. This billing software solution also offers robust reporting capabilities, enabling healthcare providers to analyze trends and make informed decisions about their practice. Contact CollaborateMD today to schedule a demo and see how this platform can benefit your practice.




